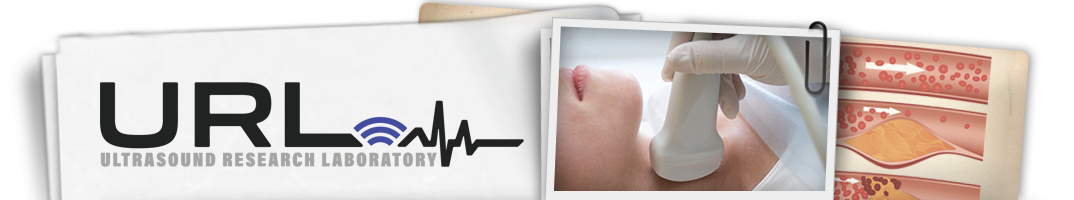
One in three women in the United States dies of heart disease, and preventing those deaths motivates Pittsburgh researchers, including Rebecca Thurston at University of Pittsburgh School of Medicine.
Just back from the international annual meeting of menopause researchers in Prague and the meeting of the North American Menopause Society in Orlando, Fla., Ms. Thurston said the challenge is sorting out early warning signs during a woman’s midlife that signal she is at risk of dying from heart disease in the future.
Traditional risk factors for cardiovascular disease, such as high cholesterol, high blood pressure and obesity, apply to both men and women. Other factors, though, are believed to be more important in setting the stage for disease in women. These include diabetes, mental stress and depression, smoking, inactivity, menopause, sudden heart muscle failure from stress and complications from pregnancy.
Within the period of menopause — which marks the end of menstrual cycles and when estrogen levels are low — research is digging into the seriousness of symptoms, such as hot flashes and sleep problems, that affect most women years before heart problems arise.
“We don’t always do so well with women in early prevention,” Ms. Thurston said. “That’s the time to intervene, the earlier the better. … We think about midlife markers for women, particularly vasomotor symptoms [such as hot flashes]. Who are these women we should really look out for?”
Ms. Thurston, who holds a Ph.D. in clinical health psychology, was awarded this year’s Henry Burger Prize from the International Menopause Society for her contributions to the field of menopause science. She’s author of several recent studies probing links between hot flashes and sleep problems and the development of cardiovascular disease, often starting with plaque buildup in blood vessels and poor blood flow to the heart and other parts of the body.
“Oftentimes, in women’s 40s and 50s, they are a good 20 years from a clinical event [such as a heart attack].” She said advances in prevention haven’t been as successful for women as they have for men.
She was lead author of a recently published observational study of 254 women with signs of ischemic heart disease, which found a link between vasomotor symptoms in early menopause and the risk of dying of heart disease.
The relationship between sleep problems and the buildup of plaque in the carotid artery was studied in a paper released Oct. 5 at the Orlando meeting. The study followed a group of 256 perimenopausal and postmenopausal women ages 40-60 for three days, with an activity monitor measuring sleep inactivity. Data was also collected from 24 hours of skin hot-flash monitoring, questionnaires and measurements of blood and the carotid artery. Results were analyzed by taking out hot-flash effects and heart disease risk factors, Ms. Thurston explained, and a connection was found between shorter sleep time and poorer sleep quality and thicker artery walls and layers of plaque within the artery, known as carotid atherosclerosis. The thickening of artery walls — intima media thickness, or IMT — may not cause symptoms, but over time, worsening atherosclerosis can lead to dangerously low blood flow to the brain, a cause of stroke.
Compared to women sleeping six to seven hours a night, women sleeping five to six hours showed higher numbers for thickness and plaque in the artery walls when measured by ultrasound.
“During midlife, women’s cardiovascular risk accelerates,” Ms. Thurston said, citing IMT and other markers that point to a risk of vascular disease.
“It’s not necessarily all about hormones,” she said, “What is accelerating their risk? There are multiple possibilities. Women are gaining weight more rapidly, they also have distinct menopausal symptoms, like vasomotor symptoms. For one third of women they are very severe. About half of women report problems with sleep.”
She said there is more work to be done to establish if sleep disturbances or hot flashes directly cause women’s health problems.
“Many of our models of cardiovascular disease are based on a male model. We’re doing a game of catch-up — both to characterize cardiovascular disease in women as well as its risk factors. There may be a subset of risk factors unique to women, related to pregnancy and menopausal phenomena.”
She said Pitt researchers recently received $3.7 million from the National Institutes of Health to expand the study of the women with vasomotor symptoms and sleep problems to see if those factors also affect the health of blood vessels in the brain — which are related to the risk of stroke, Alzheimer’s disease and dementia.